Claimocity Claims
In House vs Outsourced Billing Services:
An Inpatient MD Guide to Smarter Billing Decisions

You didn’t go to medical school to master the intricacies of revenue cycle management. Yet here you are, weighing whether to keep billing in-house or hand it off to specialists. It’s an operational decision and a financial one, and it directly impacts your practice’s bottom line.
Billing is one of the few operational areas that touch every part of an inpatient practice. It affects cash flow, staffing, compliance, and how much time leadership spends managing issues that never show up on a schedule. A recent study found that practices spend an average of 15.5 hours per week on billing and insurance-related activities. Yet many groups stick with the billing model they inherited, not one they actively chose.
The landscape of medical billing has shifted dramatically. What worked five years ago may be bleeding revenue today. Between evolving payer requirements, staffing challenges, and compliance complexities, the gap between average and excellent billing has never been wider.
This guide breaks down how each model works, where each tends to perform well, and where risks often surface. The goal is not to push a default answer, but to help inpatient groups evaluate which approach supports long-term financial stability with less friction.
What Medical Coding Productivity Standards Mean
Before comparing in-house and outsourced billing, it helps to clarify what medical billing actually includes in an inpatient setting. Billing is not a single task. It is a connected set of processes, and issues at any stage can delay reimbursement or lead to denials.
What is Hospitalist Billing?
Hospitalist billing refers to the specialized process of capturing, coding, and submitting claims for inpatient services. Unlike outpatient billing, it involves complex facility fee structures, multiple payer rules, and coordination with hospital systems. Hospitalist billing requires deep knowledge of evaluation and management codes, inpatient documentation requirements, and facility-specific protocols that change constantly.
What is In-House Medical Billing?
In-house medical billing means your practice employs its own staff to manage the entire billing process. Your team handles everything from charge capture and coding to claim submission, payment posting, and denial management. You maintain direct control over the workflow, but you’re also responsible for hiring, training, technology investments, and staying current with regulatory changes. This includes charge capture, coding, claim submission, payment posting, and denial follow-up. Because inpatient providers often work across multiple facilities and systems, billing workflows tend to be more complex than outpatient or clinic-based billing. This approach keeps billing fully internal, along with the operational responsibility that comes with it.
In-house billing teams typically manage:
- Charge capture coordination
- Medical coding and claim submission
- Denial management and appeals
- Payment posting and reconciliation
- Ongoing payer communication
How does outsourced medical billing work?
Outsourced medical billing transfers your billing operations to a specialized company that handles the process from start to finish. You provide patient encounter data, and the medical billing service manages charge capture, coding, claim submission, payment posting, denial management, and patient collections. You maintain oversight through reporting and regular communication, but the day-to-day execution happens off your plate. For many inpatient practices, outsourced billing functions as a dedicated billing department without the burden of internal staffing and management.
Outsourced billing services commonly include:
- Coding and claim submission
- Denial tracking and follow-up
- Payment posting and reporting
- Monitoring payer rules and updates
What is the role of the clearinghouse in medical billing?
A clearinghouse is an intermediary that processes electronic claims and transactions between healthcare providers and insurance companies. Clearinghouses receive electronic claims from providers, verify accuracy and completeness, and forward them to the appropriate payer. They also receive electronic remittance advice from payers, which helps reconcile accounts receivable and manage denials. Types include commercial clearinghouses (privately owned), government clearinghouses (for Medicare/Medicaid programs), integrated delivery network clearinghouses (owned by healthcare systems), and specialty clearinghouses (focused on areas like dental or behavioral health).
key metrics for medical billing
Choosing between in-house and outsourced billing requires looking beyond gut feelings and sales pitches. Tracking specific metrics reveals the health of your revenue cycle. Even small differences in clean claim rate, denial volume, or days in A/R can translate into six-figure revenue gaps over time for inpatient practices. Whether you’re evaluating your current performance or vetting potential billing partners, these KPIs provide the clearest picture of what’s working and what’s costing you money.
- Clean claim rate: This measures the percentage of claims that are processed without errors or rejections. A high clean claim rate indicates efficient billing processes, and a low rate suggests billing errors that need to be addressed.
- Reimbursement rate: This is typically an internal process analytic used to evaluate the percentage of revenue collected against the total revenue possible. Industry average hovers between 85-89%.
- Days in accounts receivable (AR): This metric measures the average number of days it takes for a provider to receive payment after submitting a claim. A lower AR indicates better cash flow management.
- Collection rate: This metric measures the percentage of outstanding balances that are collected. A high collection rate indicates effective collection processes, and a low rate suggests a need for improvement.
- Denial rate: This measures the percentage of claims that are denied by insurance companies. A high denial rate can indicate issues with coding or documentation and may lead to longer AR days and lower revenue.
- Net collection rate: This metric measures the percentage of billed charges that are collected. A high net collection rate indicates effective revenue cycle management, and a low rate suggests a need for improvement.
- Average reimbursement per claim: This measures the average amount paid by insurance companies for each claim. A higher average reimbursement rate suggests that providers are charging appropriately for their services.
- Cost to collect: This metric measures the cost of collecting payments from patients and insurance companies. A lower cost to collect indicates efficient billing processes.
In-House Billing: Pros and Cons
Many inpatient practices begin with in-house billing because it offers a sense of control and familiarity. For some groups, especially those with stable staffing and simpler payer mixes, this model can work well. However, as billing complexity increases, the limitations of managing everything internally often become an overwhelming burden.
Pros
Control and customization: By handling medical billing in-house, healthcare organizations have complete control over the billing process and can customize it to their specific needs. They can also make changes quickly if needed.
Cost-effectiveness: In some cases, in-house medical billing can be more cost-effective than outsourcing to a third-party vendor, especially for larger healthcare organizations with established billing processes and the resources to invest in large billing teams.
Better coordination: In-house billing staff are more closely integrated with other parts of the healthcare organization, which can lead to better coordination and communication between departments.
Specialized revenue: In-house billing staff have the luxury of specializing in a single organization’s revenue cycle, allowing for greater familiarity that can identify and address potential revenue leaks more effectively. This can result in increased revenue and improved financial performance.
More accurate coding: With access to the charts for verification and follow-up purposes, in-house billing staff can ensure that the correct codes are used for medical procedures and services, reducing the risk of errors and denials.
Better compliance: In-house billing staff can ensure that the organization is compliant with all relevant regulations and standards, reducing the risk of legal and financial penalties.
Cons
Complexity of billing: Hospitalists provide hospital services, some of which are complex to bill and require experience and specialization. Outsourcing medical billing to a vendor with expertise in hospitalist billing may ensure more accurate coding, fewer billing errors, and faster reimbursements.
Higher overhead costs: In-house medical billing requires a significant investment in staff, technology, and infrastructure. This can result in higher overhead costs for healthcare organizations, especially small to medium practices.
Staffing challenges: Healthcare organizations must hire and train skilled billing staff to handle in-house billing, which can be expensive and time-consuming. Additionally, it is difficult to discern the successful hires from the unsuccessful hires until a significant investment has been made in time, resources, and training.
Staff churn: Staff turnover is a common occurrence in the RCM industry and can significantly disrupt the billing process and lead to errors and delays. Hiring and training replacements is a lengthy and costly process that can set the RCM and A/R processes behind by hundreds of thousands very quickly.
Technology requirements: In-house medical billing requires healthcare organizations to invest in and maintain technology such as billing software, hardware, and IT support. This can be costly and time-consuming, especially for small to medium practices.
Compliance and regulatory issues: Healthcare organizations that handle medical billing in-house must comply with (and adjust to) complex regulations and standards, which can be extremely hard to navigate and intensely time-consuming. Failure to comply can result in legal and financial penalties, audits, and liability issues.
Increased risk of errors and denials: In-house billing staff may lack the expertise or resources to effectively manage the billing process, leading to errors and denials. This can result in delayed payments and reduced revenue.
Understaffing issues: In-house teams are typically small and specialized but lack the manpower/woman power to handle the post-denial process workload, losing significant revenue to a high percentage of good claims that aren’t deemed clean on the first pass.
Limited scalability: In-house medical billing may be less scalable than outsourcing to a third-party vendor, as healthcare organizations may lack the resources to handle increased or varied billing volume.
The administrative burden scales differently depending on practice size and available resources. Research shows practices with fewer than five physicians spend approximately 15% of their total revenue on billing activities, compared to 10% for practices with more than 20 physicians. Overall, in-house medical billing can be costly and complex, requiring healthcare organizations to invest in staffing, technology, and compliance. Healthcare organizations must carefully consider the pros and cons of in-house billing versus outsourcing to determine the best option for their needs.
Outsourced Billing: Pros and Cons
For most inpatient practices, outsourced billing delivers better financial outcomes while freeing up resources for patient care. Data consistently shows higher collection rates, lower costs, and faster reimbursements compared to in-house operations. Here’s what you need to know about making the switch.
Pros
Reduced administrative burden: Outsourcing medical billing and coding can reduce the administrative burden on healthcare organizations, allowing staff to focus on other areas of the practice, such as patient care.
Increased efficiency: Medical billing and coding vendors have expertise and resources to manage the billing process more efficiently, resulting in faster reimbursements and improved revenue cycle management.
Access to specialized expertise: Medical billing and coding vendors have specialized expertise in coding and compliance, which can help reduce the risk of errors and denials.
Cost savings: Outsourcing medical billing and coding can result in cost savings for healthcare organizations, as it eliminates the need to hire and train specialized billing staff and invest in technology and infrastructure.
Improved accuracy: Medical billing and coding vendors have processes in place to ensure accurate coding and billing, which can help reduce errors and denials and improve clean claim rates.
Scalability: Medical billing and coding vendors can handle increased billing volume, which may not be feasible for in-house billing staff.
Specialty expertise: Medical billing and coding can be complex and require specialized expertise. Outsourcing to a vendor with expertise in medical billing and coding can ensure accurate coding, fewer billing errors, and faster reimbursements.
Faster and higher reimbursements: Outsourcing can offer revenue gains in terms of faster reimbursements and better pass-through rates, which lead to reduced follow-up processing costs.
Better support: Outsourcing offers a much higher level of professional support than an in-house billing team can provide, which may impact coding, accuracy, and billing efficiency.
Compliance and regulatory expertise: Medical billing and coding are subject to complex regulations and standards. Outsourcing to a vendor with expertise in compliance and regulatory requirements can help reduce the risk of legal and financial penalties.
Access to advanced technology: Outsourcing to a vendor can provide access to advanced billing and coding technology that may be too costly for smaller practices to invest in and maintain in-house.
Reduced risks: Outsourcing billing puts the onus of data protection and security on the billing company, adding a layer of protection against risk.
Cons
Less direct control: Outsourcing medical billing and coding means that a third-party vendor is handling a critical part of the revenue cycle management process. This can result in less minute-to-minute control over the process, though quality vendors give robust reporting and regular communication.
Communication considerations: Outsourcing requires establishing clear communication channels between your healthcare organization and the vendor. Setting expectations up front helps prevent delays in resolving issues or addressing billing questions.
Importance of transparency: Choosing a vendor with financial transparency is critical. Look for billing companies that provide detailed reporting and clear visibility into performance metrics, so you can track results and hold them accountable.
Vendor evaluation: Healthcare organizations should thoroughly evaluate potential vendors’ track record, reputation, and client references before deciding. The quality of the outsourced billing company matters significantly to your outcomes.
In-House vs. Outsourced Billing at a Glance
At a high level, the difference between in-house and outsourced billing comes down to how your operational risk is managed and what workload you and your team are able to handle.
In-house billing offers:
- Direct internal oversight and control
- Familiarity with your specific practice workflows
- Full customization of billing processes
- Dependence on internal staffing and systems
Outsourced billing offers:
- Specialized billing and coding expertise
- Consistent coverage and scalability without hiring
- Reduced operational strain on your practice
- Advanced technology without capital investment
For many inpatient practices, outsourced billing provides greater stability as billing complexity and volume increase.
Take a look at the data side-by-side:
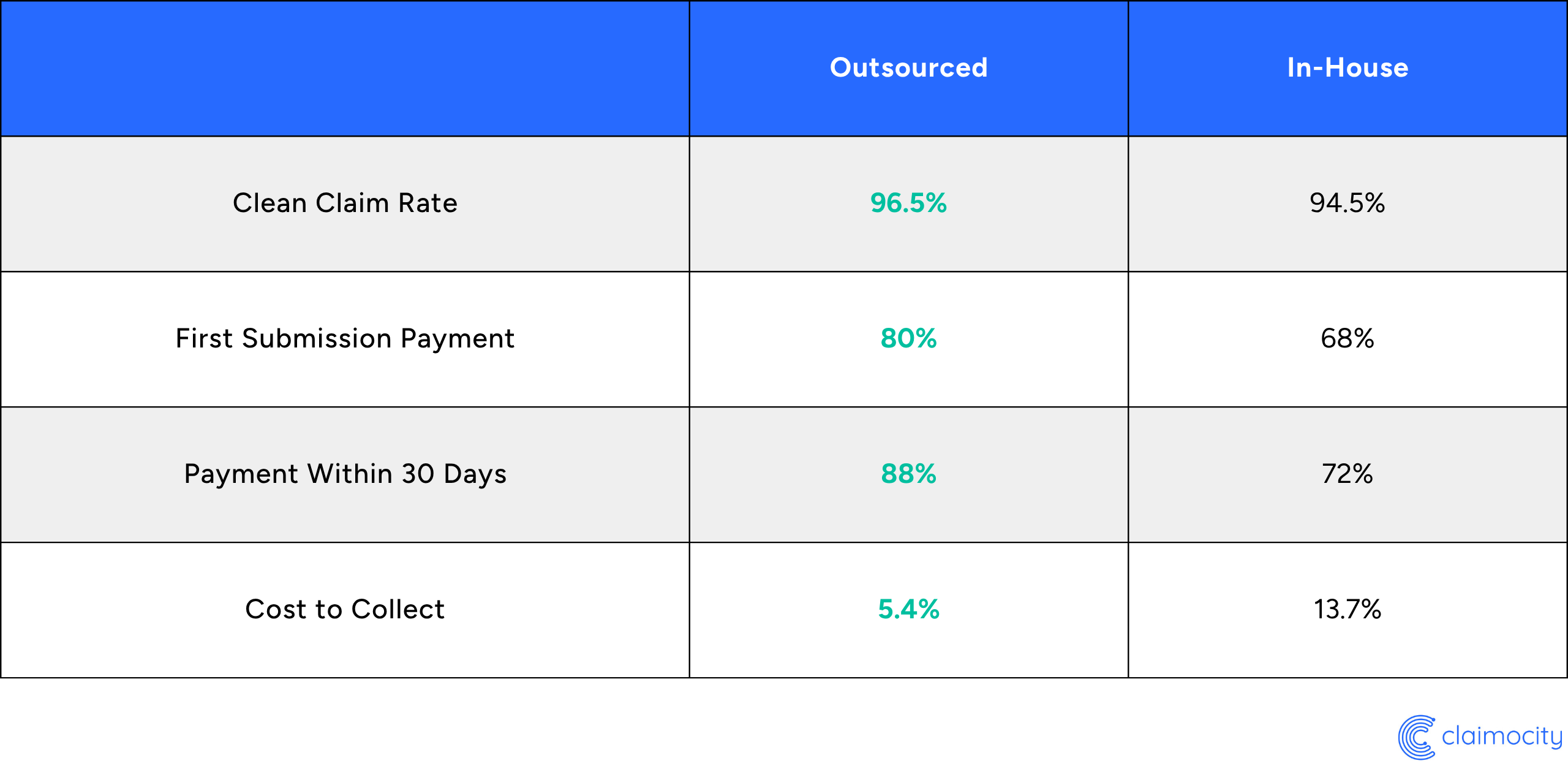
The Bottom Line
Both approaches can work, but the outcomes can be very different and your choice depends on your priorities. In-house billing tends to make the most sense for large organizations with dedicated billing leadership, stable staffing, and the infrastructure to absorb ongoing compliance and technology demands.
In practice, many inpatient groups operate under tighter constraints. Staffing turnover, rising overhead, and shifting payer rules make it harder to sustain consistent billing performance internally. Outsourced billing addresses these pressure points by providing specialized expertise, built-in coverage, and the ability to adapt as billing volume and complexity change.
Billing decisions tend to feel theoretical until something breaks. When denied claims pile up, a key staff member leaves, or payments slow down, billing quickly becomes a daily concern instead of a background process. At that point, the structure behind billing matters just as much as who is doing the work.
Trends in Outsourced Billing
Outsourced medical billing has evolved over the past several years. What was once viewed primarily as a cost decision is now more often about reliability, coverage, and the ability to keep billing running smoothly as requirements grow more complex. These trends show why outsourced billing continues to gain market share while in-house operations struggle to keep pace:
More Specialization By Care Setting
Billing companies are moving away from broad, one-size-fits-all models. Inpatient-focused teams bring a clearer understanding of hospital workflows, facility rules, and payer expectations.
A Shift Toward Preventing Denials Earlier
Instead of focusing only on appeals, outsourced billing services are putting more attention on front-end accuracy, documentation review, and staying current with payer changes.
Adoption of Technology and Automation
Centralized reporting, claim tracking, and performance dashboards make it easier for practices to see what’s happening without digging through spreadsheets or chasing updates.
Closer Coordination Between Billing and Credentialing
More practices are looking for partners that can align credentialing, enrollment, and billing, reducing avoidable claim delays tied to provider status issues.
Strategies to Reduce Denials
Reducing claim denials is one of the fastest ways to improve your revenue cycle, and denials usually point to underlying issues in your workflows. Documentation gaps, credentialing mismatches, payer rule changes, and delayed follow-up all contribute to avoidable denials over time. Studies show that 86% of claim denials are preventable, yet most practices lack the right approach to address them. Reducing your denials requires a proactive approach, with stronger front-end accuracy, clearer ownership of follow-up, and regular review of denial patterns. For a closer look at how inpatient practices address these issues, take a look at our analysis of denial management strategies and trends in revenue cycle management.
How Much Does Outsourced Billing Cost?
Outsourced medical billing is priced differently than in-house operations, which can make side-by-side comparisons less straightforward. Instead of salaries, benefits, and internal systems, costs are typically tied to collections or the scope of services provided.
Most outsourced billing arrangements fall into one of two structures:
Percentage of Collections
Medical billing companies commonly charge a percentage of a practice’s collections. For inpatient billing, this percentage typically falls between 5 and 10 percent, depending on volume, payer mix, and billing complexity.
Flat Fixed Fees
Other vendors offer fixed monthly pricing or per-encounter rates. This approach can provide cost predictability, but it’s important to understand which services are included and which may be billed separately. They are designed to be proportional to the contracted rate, but end up coming out of the collected rate. For example, a contracted rate of $100, keeps the $4-10 flat fee at the same 4-10% range, but actual collections are often below the contracted rate, so if the actual collection is $78, then the $4-10 flat fee balloons to 5-13% per claim.
When evaluating cost, the percentage itself is only part of the picture. Billing performance, denial rates, follow-up rigor, and the amount of internal oversight required all affect what that percentage really represents over time. A lower rate does not always translate to better financial outcomes if collections suffer or internal effort increases.
For most inpatient practices, the goal is not to secure the lowest possible percentage, but to align cost with consistent performance and reduced operational strain.
13 Tips for Choosing the Right Medical Billing Solution
Choosing a billing partner comes down to a few things. The right fit depends on experience, transparency, and how well a vendor supports your day-to-day operations.
Here are some thoughts to consider:
- Features: Consider what features the medical billing solution offers and whether they align with your needs. Look for features such as claims management, patient billing, claims tracking, patient eligibility verification, payment processing, denial management, and reporting.
- Ease of use: Choose a medical billing solution that is easy to use and intuitive for your staff. This can help reduce errors and increase productivity.
- Integration: Look for a medical billing solution that can integrate with your electronic health record (EHR) system, practice management software, and other tools you use in your practice. This can help streamline your billing process and improve accuracy.
- Customer support: Ensure that the medical billing solution you choose offers strong customer support, quick response times, personalized service, and training resources to help you and your staff navigate the system.
- Cost: Consider the cost of the medical billing solution and whether it is within your budget. Be sure to factor in any additional costs, such as implementation, training, and ongoing support.
- Security: Ensure that the medical billing solution you choose has strong security measures in place to protect sensitive patient information.
- Reputation: Look for a medical billing solution with a good reputation in the industry and positive reviews from other healthcare providers.
- Referrals: It may also be helpful to consult with colleagues or industry experts for recommendations and insights.
- Initial A/R audit: This won’t help in the decision process, but a clear indicator of both the quality of the new billing vs the quality of the old billing is the amount of A/R they can process and save from expiring that was left unprocessed and expiring by the prior option.
- Compatibility: Ensure that the billing solution is compatible with your existing electronic health records (EHR) system or practice management software. This will help to streamline the billing process and reduce the risk of errors.
- Specialty-driven: Some systems work well for some specialties and poorly for others. Hospitalists in the past have been forced to utilize billing and PM software that wasn’t designed for their needs, resulting in paying premiums for fractional value.
- Compliance: Verify that the billing solution complies with all relevant regulatory standards, such as HIPAA and CMS regulations. This will help to ensure that your organization is compliant and help reduce the risk of penalties or fines.
- Scalability: Consider the ability of the medical billing solution to scale with your organization’s needs, including adding new providers or services.
How to Transition Without Friction
A billing transition is a process, not a handoff. Planning ahead, clear communication, and ongoing review tend to make the difference between a smooth switch and a frustrating one.
Prepare Workflows Ahead of Time
Document current billing processes, data sources, and reporting needs before the transition begins. Clear inputs help avoid gaps once responsibilities shift.
Communicate With Staff Early
Providers and their teams should understand what’s changing and how the transition will work. Clarity early on in the process helps maintain day-to-day continuity.
Set Performance Benchmarks
Define how success will be measured using metrics like clean claim rate, denial trends, and days in A/R. Shared benchmarks create accountability from the start.
Plan for Ongoing Review
Treat the transition as the beginning of a partnership, not a one-time event. Regular check-ins and feedback help billing performance stay aligned as needs evolve.
Strong partnerships require ongoing feedback from both sides. Your billing partner should share insights about coding patterns, payer trends, and documentation opportunities. You need to raise concerns and ask questions without hesitation. This back-and-forth keeps the relationship working for your practice.
At Claimocity, we’ve guided hundreds of practices through transitions with minimal revenue disruption. Our implementation team stays involved throughout the process to address issues as they come up. For a detailed roadmap of what to expect, read our complete guide to switching medical billing services.
Partner With Billing Experts Who Understand Inpatient Care
Billing shouldn’t be the thing that keeps you up at night or pulls your focus from running your practice. At Claimocity, we’ve spent over 20 years working exclusively with inpatient providers, which means we understand the specific challenges hospitalists face. Complex facility billing, multiple payer requirements, credentialing coordination, and the constant pressure to maintain cash flow while managing everything else.
Our approach is built around partnership, not just processing claims. We work alongside your practice to optimize your revenue cycle, reduce administrative strain, and give you visibility into performance without adding to your workload. Whether you’re evaluating your current billing setup or ready to make a change, we can show you what’s possible when billing actually works the way it should.
Wondering if your current billing approach is holding you back? Talk to our team about where you are now and where you want to be. We’ll show you what’s possible when billing actually works for your practice instead of against it.


