
A Guide to Effective Medical Practice Management
Read about essential tips on managing a medical practice, from billing optimization to compliance and leveraging the latest technology for better workflows.
According to research published in Health Affairs, hospitals in the U.S. spend nearly $39 billion a year managing billing and insurance-related work. On top of that, about 1 in 5 medical claims are initially denied, which creates extra work and delays payment. For inpatient providers, this is more than just an administrative issue. It directly affects staffing, cash flow, and the amount of time teams can spend on patient care.
The difficulties are compounding. Compliance requirements are updated regularly, often adding complexity to billing processes. For years, the industry has experienced a staffing shortage, which can be attributed, in large part, to burnout from ever-increasing admin responsibilities. So, how can an inpatient provider control operational costs while maintaining revenue integrity and compliance without adding headcount in an industry of ever-shrinking margins?
Many organizations are taking a closer look at their billing approach and asking a simple question: how much does it actually cost to outsource medical billing? The answer is not always straightforward. It depends on how your organization operates, how complex your claims are, and what services you need. For many providers, the real decision comes down to whether it makes more financial sense to keep billing in-house or partner with an outside team. Understanding the true cost on both sides is the first step toward making a confident choice and helping healthcare providers make informed decisions.
Core pricing structure and scope have a lot to do with the overall expense of outsourced medical billing. The scope of services provided, whether you only need coding services or you need full RCM, significantly impacts the cost. The various pricing models also need to be taken into account. Different services use percentage-based fees, flat fees, per-claim fees, or hourly pricing. The size and scale of your practice also affect the cost. For example, large, enterprise-level hospital systems may be able to negotiate lower percentage rates, but they may also face minimum monthly fees.
Other factors that impact outsourced billing are related to complexity and workload. Higher inpatient acuity affects reimbursement variability and makes accurate coding more difficult. Higher denial rates and resubmissions also raise expenses and require stronger denial management workflows. Some specialty-specific needs, such as surgical, behavioral health, and acute inpatient services require specialized expertise, which affects pricing.
Technology and infrastructure can also be factors. Analytics tools and advanced medical billing software can increase costs initially, but often reduce operational expenses in the long term. EHR and clearinghouse integration complexity makes billing more complicated and can drive spend up, including additional administrative fees.
There are costs and hidden expenses associated with having your own in-house billing team. The most significant direct cost is staffing. Billing professionals, coders, and revenue cycle staff require pay. Those employees also receive benefits. Payroll taxes and retention expenses add up, as well. In the face of evolving compliance requirements and medical coding standards, your billing team will need ongoing training and certification. Other costs associated with an in-house billing team include licensing for medical billing software, clearinghouse fees, and IT infrastructure spend.
Many practices add RCM tasks into clinicians’ responsibilities. While this may seem efficient on its face, it tends to lead to another batch of problems and expenses. Burnout rates have been shown to become significantly higher when administrative tasks are added to clinicians’ already full workloads. It also leads to denial management gaps. The hidden cost of tasking clinicians with RCM is revenue leakage from coding errors and underbilling, which lead to higher denial rates and reduced and delayed cash flow.
There are several pricing models that are commonly used by billing companies. Some companies use a model that charges a percentage of revenue. Fees are based on complexity and volume of claims. This model works best for practices with high claim volumes with consistent reimbursement patterns. The advantage for providers is that this model incentivizes the vendor because their revenue is aligned with collections performance.
Some vendors charge a fixed monthly or per claim fee. The advantage is a predictable billing cost, which makes budgeting easier. However, this model may not include denial management services. This model works best for practices that mostly deal with lower complexity care or environments with stable workflows.
Another model that simplifies budgeting is the per-provider subscription billing model, which charges a fixed monthly fee based on provider count. Hybrid pricing models combine a flat fee with percentage pricing, which balances predictable cost with vendor performance incentives.
Inpatient practices often experience higher billing expenses because high acuity services increase the need for expert billing services, which can be more expensive. Also, minimum fees and contract terms often apply for outsourced billing services handling large healthcare organizations.
Generally speaking, outsourced billing reduces hidden costs and improves financial predictability. Despite the added control, in-house medical billing actually increases financial and operational risk.
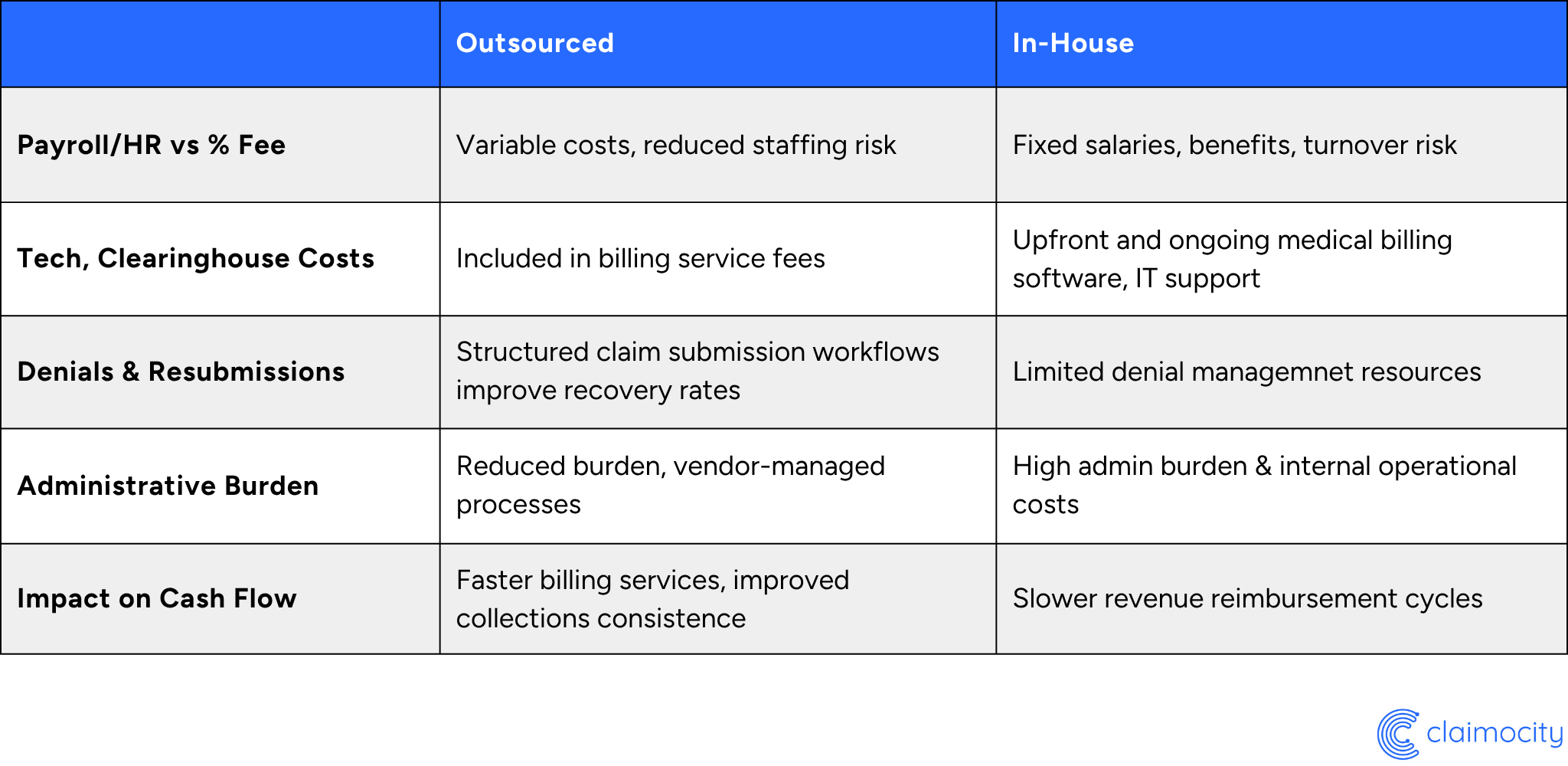
While billing is a necessary reality, it’s not the top priority for most providers when they are opening a clinic. For this reason, many practices, especially smaller ones, aren’t an ideal fit for a dedicated billing staff. That’s where outsourced billing provides an advantage. It eliminates the need and the cost of an in-house billing staff. Billing specialists also improve coding accuracy and reimbursement rates. The reduced administrative burden allows your clinicians to spend less time on repetitive documentation tasks.
Outsourced billing gives you access to advanced technology without the upfront cost of medical billing software. Scalable support aligns with your practice size and claim volume, and adapts seamlessly as your practice grows. Outsourcing also strengthens your compliance with evolving health insurance requirements and regulations.
Outsourcing billing also reduces the risks associated with hiring and managing your own RCM team. You don’t have to worry about recruiting, training, or replacing billing staff if someone leaves. Many outsourced billing services also use pricing models where they are paid based on how much they collect, which means their success is tied to your results. This shifts some of the financial risk away from your organization and gives the vendor an incentive to perform well. For a deeper look at how this works in practice, check out our blog post about the benefits of outsourcing medical billing.
Not all billing vendors are created equal. There are things you need to know before hiring an outsourced billing team. You should base your evaluation on transparency, accountability, and specialized expertise.
Here are the questions to ask before signing any contracts:
There are several benefits to outsourcing your billing, including reduced overall cost, improved cash flow, and minimized risk for inpatient providers. In-house billing teams, on the other hand, introduce hidden costs, staffing challenges, and compliance exposure. The best results for your practice will come from a dedicated medical billing company that offers transparent pricing, automation, and expert billing.
Ideally, the company you hire should tailor its billing services cost to specific services provided and claim volume. They should align to long-term revenue cycle management goals, and should be flexible enough to scale with your practice.
How much can you save when you outsource your billing and optimize your revenue cycle? Book a demo with Claimocity today to find out.

Read about essential tips on managing a medical practice, from billing optimization to compliance and leveraging the latest technology for better workflows.

Learn about how healthcare revenue integrity improves billing accuracy and reduces revenue loss, as well as how to implement a revenue integrity program.

Explore the costs and benefits of outsourcing medical billing versus in-house billing for inpatient providers.